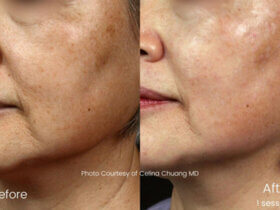
Cosmeceuticals are where beauty meets science, offering skincare products that don’t just mask problems but actively transform the skin. Packed with potent active ingredients like peptides, antioxidants, and growth factors. These high-performance formulations target ageing, acne, pigmentation, and more at a deeper cellular level.
To further explore the effective application of topical cosmeceuticals, we turn to the expertise of Dr Manasi Shirolikar, Consultant Dermatologist and Founder of online consulting brand Dr.manasi.skin.
In conversation with AMI Editor Shriyal Sethumadhavan, she discusses a complete approach to selecting topical cosmeceuticals for patients, enhancing understanding in clinical practice.
What are the key factors dermatologists should consider when choosing topical cosmeceuticals for their patients?
A thorough patient history is essential to provide them with a balanced skincare routine using cosmeceuticals.
For example, some patients are allergic to topical vitamin C, while others cannot handle benzoyl peroxide. We need this information beforehand. It’s also crucial to know what products they may or may not have tried previously, and whether those products worked for them.
Next, we need to understand their skin type. For instance, if someone has extremely oily skin, we would not recommend heavy formulations. We also need to consider if they have sensitive or acne-prone skin, so we can tailor their routine accordingly.
Another critical aspect is compliance. If we want to prescribe even a basic three- or four-step routine, but the patient is not likely to follow through, it does not make sense. Knowing their general routine is important too. For example, if the patient works night shifts, we would adjust their routine accordingly.
When selecting cosmeceuticals, we also consider the ingredients and the delivery system — whether it is a serum, moisturizer, or emulsion. We take all of these factors into account before recommending cosmeceuticals.
Can you highlight the most common active ingredients in cosmeceuticals and their specific skin benefits?
One of the most common ingredients is hyaluronic acid. As we know, it’s a humectant that holds up to 1,000 times its weight in water. It is particularly beneficial for skin that cannot tolerate exfoliants or vitamin C, as it hydrates the skin. If a person has a compromised skin barrier with significant transepidermal water loss, hyaluronic acid can be helpful.
Then there is niacinamide, which is beginner-friendly and suitable even for sensitive skin. It hydrates, brightens, and helps regulate sebum production, making it beneficial for oily and acne-prone skin.
Retinoids have been around since the 1980s. We now have different formulations like retinol, retinyl palmitate, and retinaldehyde, which are available over the counter. Retinoids promote skin cell turnover, stimulate collagen synthesis, and help reduce fine lines and prevent deeper wrinkles.
They also aid in retaining water, giving the skin a plump, glowing look. Additionally, they help with acne. Adapalene, for example, is a prescription retinoid that effectively treats acne.
Vitamin C is another powerful antioxidant, although it’s known to be unstable. We try to stabilize it with ferulic acid and vitamin E. Vitamin C supports collagen synthesis, fights free radicals, reduces pigmentation, and fights signs of aging.
We also have exfoliants like AHAs and BHAs. AHAs dissolve the upper layers of the skin, helping with pigmentation and texture, while BHAs penetrate deep into the follicles, unclogging them and preventing acne formation.
Finally, peptides are gaining popularity. They help with brightening and have anti-aging benefits, though research on peptides is still evolving. They’re often combined with vitamin C or retinoids in formulations.
Are there any challenges in integrating cosmeceuticals into treatment plans for different skin types, especially for sensitive or acne-prone skin?
With sensitive skin, we avoid anything that could impair the skin barrier. We opt for gentler products. Instead of AHAs, we might use azelaic acid or a milder AHA like lactic or mandelic acid, in lower percentages.
Instead of salicylic acid, we could use betaine salicylate, which is gentler. Niacinamide is another option as it helps without triggering barrier damage. For acne-prone skin, we avoid oil-based formulations, favouring water-based, non-comedogenic products.
It is important to moisturize acne-prone skin because dry skin can lead to increased oil production, clogging follicles and causing breakouts. So, we use oil-free moisturizers with ingredients like hyaluronic acid.
Post-inflammatory hyperpigmentation is a major concern for patients, as the pigmentation can last weeks or months, so incorporating treatments that address both acne and hyperpigmentation is essential.
Do cosmeceuticals complement in-office treatments like chemical peels and lasers? Are there any specific combinations that work best?
Absolutely. For in-office treatments like peels or lasers, we prep the skin beforehand. For example, if we are doing a Q-switched Nd laser treatment, we might use kojic acid, hydroquinone, or tretinoin beforehand to reduce pigmentation and promote skin cell turnover. Using AHAs before treatments can also improve results by removing the upper layers of skin, allowing the laser to work more effectively.
Post-treatment, we focus on barrier support with ingredients like ceramides, peptides, and hyaluronic acid. After peels, gentler products like azelaic acid can help with pigmentation. Niacinamide is a great post-peel option for reducing sebum production and strengthening the barrier.
With the market flooded with options, how do you differentiate between high-quality cosmeceuticals and those making exaggerated claims?
First, we need to scrutinise the claims. Products that promise no preservatives, for example, are often unrealistic because it’s impractical to finish a product in just a few days. We also check the ingredient list—if a product claims brightening or sun protection but only contains essential oils, it’s not going to deliver the promised results. Some sunscreens, for instance, claim SPF 50 but only contain carrot seed oil, which has an SPF of around 7.
Another way to differentiate is by looking for clinical data. High-quality companies will have clinical studies or trials, even with a small group of subjects, showing their product’s efficacy.
Some brands display their SPF certificates on their websites, and many will have patents or third-party trials, which are strong indicators of quality.
When consulting patients, you manage various expectations about treatment timelines, outcomes, and cosmeceuticals. How do you approach and address these expectations effectively?
First and foremost, we need to establish a clear timeline for the patient because they often come without any reference. While I’d love to tell a patient, “You need to wait 12 weeks,” and have them just accept it, it doesn’t work like that. We must explain how a product works, its mechanism of action, and how long it takes to show results.
Take an acne patient, for example. They may not only have active acne but also post-inflammatory hyperpigmentation (PIH), scarring, and possibly fine lines or wrinkles. You must provide a structured plan, and I typically start by addressing the acne first. While they may have other concerns, we can’t tackle everything while there’s active inflammation.
To address their other concerns, I might add an AHA or azelaic acid for pigmentation. By the fourth or sixth week, when they start seeing acne results, they’re usually more satisfied. They’re also more willing to wait another 8-12 weeks for pigmentation improvements before moving on to treat fine lines and wrinkles. By three to four months, with the right products, improvements are visible.
Patient awareness and compliance are essential, and you must also consider their preferences when adjusting routines. Transparency about treatment timelines ensures realistic expectations.
Could you tell us more about the role formulation stability plays in the effectiveness of cosmeceutical products, and how do you advise your patients on this?
Regarding formulation stability, let’s take L-ascorbic acid as an example. We know it’s highly unstable. If my patient is using vitamin C, I’d prefer they use L-ascorbic acid, especially for those who don’t have sensitive or acne-prone skin, and particularly for more mature patients or those with melasma or extremely dry skin.
Since L-ascorbic acid is unstable, it must be co-formulated with ingredients like vitamin E and ferulic acid to stabilise it. Packaging is equally important; it should be in an opaque bottle, not a transparent one, to prevent oxidation.
Ideally, it should be in an airless pump to avoid further oxidation from droppers. Formulation stability depends on packaging, the percentage of active ingredients, and co-formulation. Patients should also follow any specific storage instructions for such products.
Do you tailor cosmeceutical treatments for patients with different ethnic backgrounds and skin concerns? If so, how do you approach that?
Absolutely. For example, I have patients from different regions across India, and their skin types can vary significantly. If I have a patient from Kashmir, they typically have a lighter skin tone, falling into the Fitzpatrick Type II-III range. They’re more likely to experience post-inflammatory erythema (PIE) than hyperpigmentation (PIH). You’ll see more red spots rather than brown ones, so I would tailor their routine accordingly—perhaps with niacinamide or azelaic acid.
On the other hand, patients with darker skin tones who are prone to PIH would benefit more from ingredients like glycolic acid or kojic acid, which are better for treating pigmentation. Caucasian skin, for example, tends to develop PIE rather than PIH, so your product choices should reflect that.
When it comes to procedures, something like an IPL works better for erythema than for pigmentation. For patients with lighter skin, we have to be more cautious with high-potency products because they’re more prone to irritation and burns, whereas Fitzpatrick Types IV and V are more resilient. So, tailoring the treatment to the patient’s skin type and concerns is essential.
For more expert insights into the world of aesthetics, join Aesthetic Medicine India’s exclusive AM MedTalk every Sunday at 11 AM, only on Instagram @aestheticmedindia
If you missed joining us live, we have got you covered. Click here for the video: https://www.instagram.com/reel/C_7VW5TJ_ww/