As aesthetic medicine practitioners, do you believe that medico-legal issues and the law are unimportant in running your business? Or that your field is immune because patients love you? What happens when you receive a negative Google review?
It is time to take law seriously – your practice, growth, sales, and marketing teams must understand that we operate in a country governed by law, serving an educated, aware clientele who research your credentials – and even your medico-legal history – before choosing you.
Digital awareness and legal exposure
There are numerous AI tools today that guide patients on the medicines prescribed by doctors. We often say that if you have come to a lawyer, there is also another one – Google Baba –because it offers free gyan.
Nevertheless, like every other medical branch – whether it is dentistry, dermatology, cosmetic, or aesthetic – medico-legal cases are rising across India. This is primarily because patients are becoming more informed, and that is something you cannot control. You can no longer expect an uninformed patient.
From now on, you will only encounter educated, well-aware patients who know what they want – your business must be built around this reality.
Consent forms and legal documentation
I have seen well-known cosmetologists and dermatologists using Xeroxed consent forms – unclear, poorly drafted, not in the local language or proper English. I feel they are the ones who need serious introspection. Aesthetic medicine involves medical procedures aimed at improving physical appearance and patient satisfaction, using non-invasive to minimally invasive cosmetic techniques.
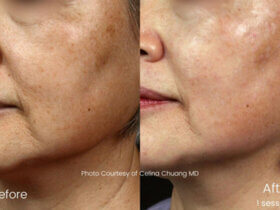
What I want to highlight is physical appearance. It is a critical part of one’s personality. When something goes wrong with a patient’s appearance, it hurts deeply – “I used to look good, now I don’t, because of a botched procedure.”
Recently, a well-known chain had an incident where a laser machine caused a cut. A 57-year-old man went for treatment. The doctor recommended a laser, but it malfunctioned, leaving a cut. I saw the before-and-after photos. He did not look like Tom Cruise – he had pigmentation, dark skin, and signs of alcoholism. The cut blended into his skin tone. Technically, at his age, it should not have mattered – retirement age in India is 58.
Still, he sued the doctor for Rs 50 crore. The procedure cost only Rs 16,000. Of course, the court will not award Rs 50 crore, but the expectations and perception matter. At 57, with settled children, no loans, no liabilities – he still demanded Rs 50 crore. There is no logic in such cases.
Patients can claim any amount. That is why in aesthetic, cosmetic, or dermatology – any field related to appearance – you must be extra cautious. You are dealing with people’s looks.
The client base is largely female – a sensitive demographic. If that man could sue for Rs 50 crore, imagine a woman – maybe ₹100 crore. You never know. Women are more particular, and sociologically, in India, there’s huge pressure to look good.
We have problematic attitudes – fair vs dark skin, North vs South, East vs West. These comparisons mess with people’s psychology. If a girl isn’t getting married, families first send her to a gynaecologist, then to a skin doctor. These societal expectations put pressure on women – and on doctors – because competition is growing and outcomes matter.
Emotions drive litigation
Human emotions linked to appearance are one of the key triggers for medico-legal cases – high expectations from treatment outcomes, pressure to look good, and the perceived cost of treatment.
Now, I don’t think cost matters as much – your treatments are not exorbitantly priced. But yes, you may have machines or equipment for which you charge. Still, cost is the last factor. Emotional factors are the biggest reason patients decide to knock on the court’s door. Let’s be clear – the trigger is almost always emotional.
For instance, I am handling a case before the Medical Council for a senior doctor from your industry. He was sued four to five times. The reason? A couple of patients found him arrogant. That perceived arrogance, combined with a couple of treatment mishaps, led to litigation.
That is why emotional factors matter just as much – if not more – than your marketing or treatment results. These emotions can be powerful legal triggers.
Medical complications and legal risk
Here are some common complications – not an exhaustive list, but drawn from my research:
- Hematoma after facelift
- Seroma post-tummy tuck
- Blood loss, infections, nerve damage post-surgery
- DVT, pulmonary embolism
If you are a surgeon, you must take these risks seriously. There have been cases where doctors did not conduct basic pre-op tests – like the D-dimer for clotting. We recently saw a botched hair transplant case – I am handling that case, where the patient died, and the doctor was suspended.
Let us be clear – surgical procedures come with greater risks than non-surgical practices.
Surgical responsibility and documentation
Surgeries are serious. Pre-operative procedures and tests are absolutely essential. Follow preventive practices – do not skip any procedural or pre-surgical checkups. Ask patients to do everything required. Do not leave anything out. I promote defensive practice for a simple reason: When a case lands in court, the first thing the judge asks is, “What did you do? Show us.” Sympathy is always with the patient.
Consumer courts are designed for consumers – you are the service provider. The court will not sympathise with you. So, we have to go the extra mile to convince the judge: “Look, I did everything I was supposed to do.” And to prove that, you must conduct all the tests you believe are necessary. Anaesthesia-related complications can also happen, including anaesthesia deaths. Anaesthesia is the most unpredictable part of any medical procedure.
Your choice of products also matters. This ties directly to your professional code of ethics, as issued by the Medical Council of India, now governed by the National Medical Commission.
When you endorse or publicly support a particular product or brand, you must remember: You are a doctor. You are not allowed to promote or endorse one specific brand openly – that is a violation of your professional code of ethics.
That is why we now advise you to prescribe only the molecule on prescriptions, not specific brand names. You must maintain autonomy in treatment choice.
New guidelines and social media conduct
The new Code of Ethics will be released soon. It has been in the drafting stage for the last three years, with multiple stakeholders and associations submitting their feedback. This time, the guidelines will also include detailed rules for social media usage.
That is why I began by asking – do you think law is important? Why do business consultants avoid including legal aspects in their presentations? Because once they implement the updated Medical Code of Ethics, it will include detailed social media guidelines: how to use it, what to post, what not to post, and the need for proper consent before showcasing surgeries or procedures.
Currently, Clause 6 of the Code of Ethics (Advertisement Rules) prohibits doctors from doing anything that invites public attention. When you upload an Instagram video, you are inviting attention. That’s a violation.
You can refer to the existing Professional Code of Ethics, 2002, even applicable to my profession. That is why I rarely use Instagram, and when I do post, it is only on LinkedIn – and that too, occasionally.
But Instagram has videos, products, hands-on visuals – all of which constitute a direct violation of your code. So how will you resolve this conundrum? It is a clear conflict between legal compliance and marketing strategy.
If someone is recommending Instagram, Facebook, or social media content creation, I suggest you wait for the new guidelines. See what they contain, and then plan accordingly. Only a medico-legal lawyer can guide you here, because this is not taught in MBA programmes.
The law is taken lightly by many in this country. But when the long arm of the law catches up, it hits hard. Prevention is always better than a cure. One medico-legal case can ruin the reputation you have built over the years.
You may not suffer financially – your professional indemnity insurance may cover the compensation. But if your name appears in the newspapers, the damage to your reputation is irreversible. So always involve a lawyer in your strategy – before it is too late.
The power of informed consent
Informed consent is the most important document you must prioritise in your practice. It is the one document that can protect you from everything. What’s peculiar in your industry – especially aesthetics – is that consent is not given enough importance. I have seen extremely poorly drafted consent forms from your sector.
Consents must evolve with time. New judgments, legal developments, and cases from the Supreme Court or National Commission keep emerging. Plus, your medical science is not finite – it is not like physics or math – it evolves constantly.
So every time your field evolves, you must check: Is my consent form still appropriate? That’s your responsibility.
One standard consent form for all treatments is no longer acceptable. Courts have said this – not me. You cannot use one generic consent form in English, Hindi, or Marathi and claim it’s sufficient.
If a patient comes for botulinum toxin, the consent must be specific to it. If it is for a filler or a jab, the consent must be different. This is a major oversight in many clinics. Several associations – gynaecologists, radiologists – have developed standardised treatment-specific consent forms available on their websites. Your industry should do the same. It ensures commonality, clarity, and legal strength.
Also, do not take medical history lightly. Record it properly before any procedure. Even a minor injection can go wrong if the patient is diabetic or has comorbidities. In many cosmetic dentistry cases, I have seen no mention of whether the patient is a smoker or an alcoholic, both of which are medically significant. For example, implants may fail if the patient is a smoker. So again – record everything.
Even minor errors in procedures can lead to legal trouble. There have been rare but shocking cases – a renowned orthopaedic surgeon operated on the wrong foot. Delayed diagnosis or failure to treat complications in time can result in litigation. Timely diagnosis and proper treatment are critical.
And patients today have high expectations. They are well-informed and tech-savvy. So, managing expectations is key. Also, never exaggerate. Give them a realistic picture of the treatment. Speak the truth, even if competition is high – your honesty will make you stand out.
Exaggerated claims on brochures, websites, or Instagram can become evidence in court.
In medico-legal complaints, patients often start by quoting claims: “This hospital says it is NABH-accredited,” or “It has world-class equipment,” – then they demand, “If everything is world-class, how did this go wrong?”
The legal foundation of negligence
Now, what is negligence? In negligence, there are four core aspects. The entire scope of medical negligence revolves around these four points – nothing beyond them.
If someone brings an action for medical negligence, the first thing the complainant (i.e., the patient) must prove is that the doctor had a duty of care toward the patient. This means the patient was officially under your care – registered with you, had filled out your forms, and paid your consultation fees. If the treatment was offered free of cost, then it is not considered a commercial transaction. Always remember: if you accept even Rs 1, you become a service provider, and the patient becomes a consumer. But if the treatment is absolutely free, the law does not recognise the relationship as commercial, and the Consumer Protection Act does not apply.
Once you have a duty of care, the next element is breach of duty. A breach happens when there is a deviation from the standard procedure. For example, liposuction is an established treatment – it may use newer machines, but the basic process remains the same. If you knowingly deviate from a recognised procedure, or attempt something experimental without standard backing, and something goes wrong, that becomes a breach of duty. So always follow standard protocols – whether from journals, SOPs, textbooks, or peer-reviewed references.
Next is causation. The breach must be directly responsible for the damage. For example, I shared the case of the laser cut – the court held the doctor responsible because he owned and operated the machine. The injury had a direct connection to the doctor’s actions.
But if the outcome is unrelated – say the patient gets cured but later develops an issue elsewhere or ignores your prescription or aftercare – it does not make you at fault. One surgeon I know (he was here yesterday; I cannot name him) handled a post-op skin graft case for a model. He wrote a perfectly meticulous discharge summary. The patient ignored his instructions – no ointments, no oils. Naturally, the graft failed, and she sued him.
This was one of my first cases, and the moment I saw his handwritten documentation, it impressed me. He had recorded every detail thoroughly, as there were no EMRs back then. We showed this to the court, and it became clear that the failure was due to the patient’s non-compliance. That is what we call contributory negligence – when the patient contributes to the failure of treatment. If it is not your fault directly, there is no negligence. You are safe!
The fourth aspect is damage. If there is a breach, and that breach causes direct harm – disability, disfigurement, death, or loss of income – then it qualifies as damage. In the model’s case, we won because she did not follow the advice. But had she followed all instructions and the graft still failed, leading to loss of work and income, it would have been a valid claim. If someone’s face gets damaged and they earn a living from it, it raises a serious legal concern.
But if there’s no actual damage – just dislike for the doctor – it does not stand in court. Courts consider a case negligence only when it causes quantifiable damage.
About the author:
Advocate Amit Karkhanis is the Senior Panel Lawyer for the Union of India and Founder, Chambers of Amit Karkhanis. With over two decades of experience, Mr Amit Karkhanis specialises in medico-legal laws, surrogacy, the healthcare sector, and intellectual property rights. He was one of the foremost lawyers to practice medico-legal and surrogacy laws in India.
(This article is adapted from Advocate Amit Kharkhanis’ presentation at the Aesthetic Medicine India Conference 2025.)